
Clinical judgment is essential to prepare students for professional practice and the upcoming Next Generation NCLEX. “Think like a nurse” is a mantra repeated throughout nursing programs to develop this important thinking skill. What needs to be remembered is that clinical judgment is an outcome that cannot be taught directly.
So how do we best develop clinical judgment?
I propose a comprehensive, holistic approach to developing clinical judgment supported by the nursing literature that is much more than using the clinical judgment steps embodied in the NCSBN Clinical Judgment Action model of recognizing cues, analyzing cues, prioritizing hypotheses, etc.
Just as a practicing nurse provides holistic care to support the physical needs and the emotional and spiritual needs inherent in every human being, holistic clinical judgment recognizes that there are also three components that need to work together to develop the clinical judgment to ensure safe practice.
These three components are:
- Caring and compassion
- Knowledge use and application
- Clinical judgment framework informed by practice
1. Caring and Compassion
Tanner’s Clinical Judgment Model, a practice-based framework derived from almost 200 research articles in the nursing literature identified that correct clinical judgments are more influenced by what nurses bring to the situation than the objective data about the current patient scenario (Tanner, 2006).
In other words, the technical, clinical judgment skills of recognizing cues or noticing what clinical data is most important are influenced more by the nurse’s inwardly possesses. This includes the motivation of the nurse to provide caring, compassionate, and engaged patient care. If a nurse is stressed or burned out, they are less likely to notice (or minimize) significant cues that are collected while providing care.
Dr. Patricia Benner recognized that professional nursing care is prefaced by the nurse being compassionate to the intimate strangers (patients) that a nurse cares for (UNLV, 2021). A professional nurse embodies the spirit of the Good Samaritan who was moved with compassion to respond to the stranger who needed care.
2. Knowledge
Nursing knowledge is typically embodied by the information in textbooks that continue to grow in size with each edition. As a result, our students are swimming in a sea of infobesity!
The problem with textbook knowledge is that it is information that is abstract and decontextualized from clinical practice. To provide safe patient care, students must understand and then be able to apply what is most important.
Practice-Based Knowledge
The bigger problem is that there is an additional way of knowing as a nurse that is not communicated in traditional textbooks. To develop holistic clinical judgment, students must be aware of the knowledge embedded in and derived from clinical practice.
This level of knowledge comes with clinical experience that, unfortunately, most students do not get enough of while in school. It is imperative that educators communicate the knowledge from clinical practice and what has been learned from experience to recognize early warning signs of a patient developing a complication such as sepsis progressing to septic shock.
The knowledge derived from practice must be made visible to students just as essential information is made clear to students from the textbook.
3. Clinical Judgment Frameworks
Once the foundation has been laid with caring and embracing what it means to be a professional nurse, then using both textbook knowledge and the knowledge derived from clinical practice, the student possesses what is needed to put it all together using a practice-based framework of clinical judgment.
Since we are teaching a practice-based profession, the frameworks used to teach and develop clinical judgment must be derived and validated from clinical practice. Though there are multiple ways of thinking that a nurse uses in practice, the two theoretical practice-based frameworks that lay the foundation for clinical judgment are:
- The nursing process
- Tanner’s Clinical Judgment Model (CJM)
The Nursing Process
Just as the curriculum is leveled from simple to complex, the theoretical framework to develop clinical judgment skills must also be leveled the same way. The nursing process is a foundational and fundamental way of thinking. Still, it has limitations because it is linear and does not provide for the situated thinking in action that is the essence of clinical reasoning.
I agree with Dr. Patricia Benner, who advocates that the nursing process should be taught in only the very first semester of nursing school and then emphasize clinical reasoning skills that lead to the outcome of a correct clinical judgment (UNLV, 2021).
Tanner’s CJM is a clinical reasoning framework derived from clinical practice and is a research and evidence-based model of clinical judgment. The four clinical reasoning processes or steps that lead to the outcome of a correct clinical judgment include:
- Noticing
- Interpreting
- Responding
- Reflecting
These steps correlate with the nursing process and the six stages of the NCSBN Clinical Judgment Action Model that will be used for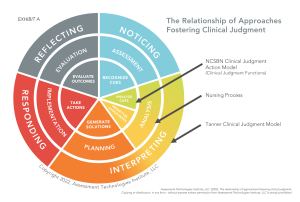 Next Generation NCLEX (NGN). Many of you might be thinking, why not teach our students the six steps of the NGN model instead?
Next Generation NCLEX (NGN). Many of you might be thinking, why not teach our students the six steps of the NGN model instead?
This infographic, used with permission from ATI, illustrates the alignment of the two practice-based clinical judgment frameworks of Tanner’s CJM, and the nursing process, with the evaluation framework of the NGN action model that is in the inner circle.
Though some advocate just that, I believe it is a mistake, and here’s why. The NGN model is a framework for measuring and evaluating clinical judgment but was never intended to guide and inform nursing practice and be taught directly to students. There is no research to support the application of this framework to practice.
Since we are teaching practice, practice-based frameworks that align with the 6 evaluative steps of the NGN action model must be introduced to students, such as the nursing process and Tanner’s CJM. The NCSBN has supported this viewpoint and encouraged the use of the six of the steps NGN action model for educators to write test questions, but it does NOT need to be taught directly to students.
New Resource
To help students understand the knowledge embedded in practice, I recognized the need to create a student-centric resource that would help translate the essence of holistic clinical judgment to the next generation of professional nurses.
The second edition of Think Like a Nurse: Practical Preparation for Professional Practice was written in 2015 and has been adopted by nursing programs and nurse residency programs across the country.
After completing my PhD in 2020, I recognized the need to update and completely revise this edition to strengthen student development of holistic clinical judgment. Over the past year, I have completed this comprehensive undertaking and am excited to share this new resource first with nurse educators!
 Instead of one single textbook, I broke this complete rewrite into three complementary volumes. Each volume captures the essence of the three components needed to develop the holistic clinical judgment that will prepare students for professional practice.
Instead of one single textbook, I broke this complete rewrite into three complementary volumes. Each volume captures the essence of the three components needed to develop the holistic clinical judgment that will prepare students for professional practice.
- Volume 1: Laying the Foundation for Professional Practice (student success/caring/professional formation)
- Volume 2: Building the Knowledge Base of Professional Practice (application of pharm/patho/F&E)
- Volume 3: Developing the Clinical Judgment for Professional Practice (Clinical judgment skills/transition to practice)
These volumes are available for purchase at an incredible discount through May 31, 2022. Reach out if you have questions or would like to consider course adoption in your program.
Curriculum Integration Map
Download a curriculum integration map to identify specific chapters in each volume that would provide a practice-based perspective on essential content/knowledge.
Related Articles
- Integrating Tanner’s Clinical Judgment Model in Your Teaching
- Frameworks to Teach Clinical Judgment
- Defining Clinical Judgment and Why it’s So Important
References
University Nevada-Las Vegas. Articulating Better Nursing Practices: An Interview with Patricia Benner. Retrieved from unlv.edu/announcement/articulating-better-nursing-practices-interview-patricia-benner.
Tanner, C. A. (2006). Thinking like a nurse: A research-based model of clinical judgment in nursing. Journal of Nursing Education, 45(6), 204–211.
Keith Rischer – PhD, RN, CEN
As a nurse with over 35 years of experience who remained in practice as an educator, I’ve witnessed the gap between how nursing is taught and how it is practiced, and I decided to do something about it! Read more…
The Ultimate Solution to Develop Clinical Judgment Skills
KeithRN’s Think Like a Nurse Membership
Access exclusive active learning resources for faculty and students, including KeithRN Case Studies, making it your go-to resource.




