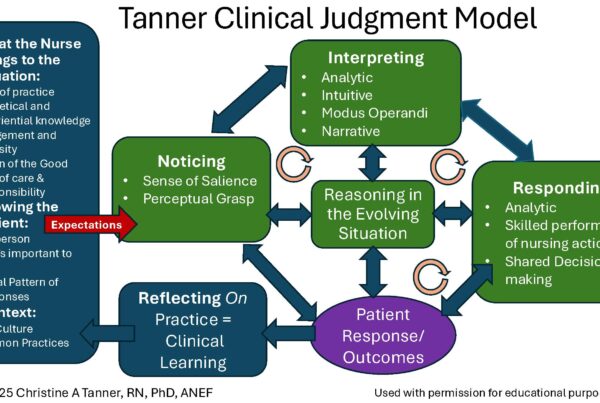
Nurse educators must create a curriculum that ensures students develop expected levels of clinical judgment to pass the NCLEX and provide safe patient care after graduation.
Many programs use predictive testing to gauge NCLEX readiness. What has been missing is an instrument to assess clinical judgment with an unfolding case study.
Since unfolding case studies that simulate clinical practice are an effective strategy for practicing clinical judgment skills, a rubric is needed that can assess and assign a quantitative score to a student’s level of clinical judgment. To accomplish this objective, one must have a solid and established foundation to build a rubric to assess clinical judgment skills using unfolding case studies.
Lasater’s Clinical Judgment Rubric (LCJR) has been used since 2007 (Lasater, 2007) and is a valid and reliable tool based on Tanner’s Clinical Judgment Model (Adamson et al., 2012; Ashcraft et al., 2013; Jensen, 2013) to quantitatively measure and assess specific clinical reasoning skills required to make clinical judgments through student performance that can be observed, using high-fidelity simulation.
Permission was obtained from Dr. Kathie Lasater, the creator of the LCJR, to adapt the LCJR, and to create the KeithRN Clinical Judgment Rubric (KRN-CJR).
What Case Studies to Use?
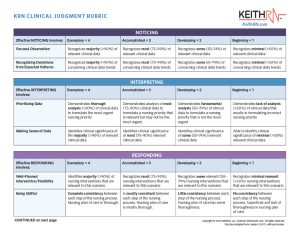 The KRN-CJR will only work with KeithRN Clinical Reasoning Case Studies because each KeithRN Case Study integrates Tanner’s CJM and uses open-ended questions to identify the level of thinking. Faculty can then assess the level of clinical judgment using salient scenarios that contextualize clinical practice.
The KRN-CJR will only work with KeithRN Clinical Reasoning Case Studies because each KeithRN Case Study integrates Tanner’s CJM and uses open-ended questions to identify the level of thinking. Faculty can then assess the level of clinical judgment using salient scenarios that contextualize clinical practice.
Assessing Clinical Judgment Step-by-Step
The four sequential reasoning steps a nurse uses to make clinical judgments addressed in Tanner’s CJM and integrated into the KRN-CJR include:
Step 1. Noticing.
Does the student notice or recognize relevant clinical data in the case study, and why is it significant? Noticing what is significant in a patient care scenario requires applying knowledge (Tanner, 2006).
Effective noticing involves the following KRN-CJR subscales:
- Focused observation
- Recognizes deviations from expected patterns
Step 2. Interpreting.
Once relevant clinical data is noticed and identified, this clinical data needs to be interpreted. What does this data mean, and what is its significance (Tanner, 2006)?
Effective interpreting involves the following KRN-CJR subscales:
- Prioritizing data
- Making sense of data
Step 3. Responding.
Responding requires the nurse to make a decision (Tanner, 2006). Based on the correct interpretation of clinical data, does the nurse need to act, respond, or continue to monitor?
Effective responding involves the following KRN-CJR subscales:
- Well-planned intervention/flexibility
- Being skillful
- Clear communication (not able to be assessed with NextGen or SKINNY Reasoning)
- Recognizing patient problems (not able to be assessed with NextGen or SKINNY Reasoning
Step 4. Reflecting.
Reflecting has two components. Reflection in action is the ability of the nurse to read the patient in the present and evaluate or adjust the nursing priority and plan of care based on the patient’s response.
Reflection on action is done afterward and is the thinking that the nurse does after the situation and reflects upon the entire clinical judgment process from start to finish (Tanner, 2006).
Effective reflecting involves the following KRN-CJR subscales:
- Evaluating plan of care
- Evaluation/self-analysis
- Commitment to improvement
Levels of Clinical Judgment: Scoring
There are four levels of clinical judgment with a numerical score that Lasater incorporated and is carried through on the KRN-CJR:
- Exemplary (4 points)
- Accomplished (3 points)
- Developing (2 points)
- Beginning (1 point)
Lasater identified that the goal for advanced nursing student performance before graduation is consistently at the accomplished level. First-year students continue to develop and would be consistently at the developing level of thinking. With a total of eleven categories and based on the performance metrics for each category, the total score for any student would range from 11 to 44.
For example, for an advanced student approaching graduation, the goal total on a case study would be around 33 points, calculated by demonstrating performance on the case study at the accomplished level (three points) for all eight subcategories (3 x 11 categories = 33).
For first-year students developing clinical judgment, you would want them to consistently be at the Developing level (2 points) for all eleven subcategories (2 x 11 categories = 22).
Scoring Worksheet
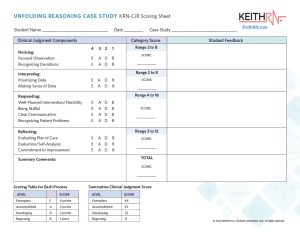 In addition to the rubric, a worksheet provides scoring and the ability to share notes and feedback with the student providing another chance for students to reflect and further strengthen clinical judgment.
In addition to the rubric, a worksheet provides scoring and the ability to share notes and feedback with the student providing another chance for students to reflect and further strengthen clinical judgment.
To help remove ambiguity regarding the levels of proficiency, for each level, use the following percentage to guide your assessment of student performance in each level:
- Exemplary = >90%
- Accomplished = appx. 75-90%
- Developing = appx. 50-74%
- Beginning = < 50%
For example, the first subcategory under NOTICING is “Focused Observation.” Exemplary performance is defined as:
- Recognizes the majority of relevant clinical data.
Since the term majority is open to interpretation, I have included the percentage >90% to remove this ambiguity. These percentages are suggested.
Scoring with SKINNY or NextGen Reasoning
The entire KRN-CJR can be used with an UNFOLDING Reasoning Case Study because it addresses all eleven subcategories of clinical reasoning.
However, if the more concise NextGen or SKINNY Reasoning level is used, the “Clear Communication” and “Recognizing Patient Problems” subcategories under the RESPONDING category cannot be assessed since these questions that align with this subcategory are not asked in the case study.
Note: These subcategories are highlighted in light orange on the rubric as a reminder. As a result, the scoring will be slightly different (see scoring worksheet doc.). When documenting the summative numerical score, the level of the case study must always be noted.
Clinical judgment can be measured and assessed using the KRN-CJR.
The KRN-CJR may provide educators with another instrument to quantitatively assess clinical judgment to ensure safe entry into practice, resulting in improved patient outcomes.
Implementation in Your Program
Remember that like the original LCJR, the KRN-CJR provides a current “snapshot” of a student’s clinical judgment development. Therefore, educators need to repeat this assessment throughout the program (at least each semester) to obtain an accurate trajectory of the student’s clinical judgment skills before graduation.
Share Rubric with Students
Sharing the KRN-CJR, in addition to a students’ scoring worksheet will allow students to see where they are currently at in their development of clinical judgment and what they need to accomplish and demonstrate to move to the next level of improved proficiency. The rubric provides an opportunity for additional reflection to strengthen their clinical judgment.
How is your program assessing clinical judgment skill development BEFORE graduation?
How could the KRN-CJR be integrated into your program to improve student assessment of clinical judgment?
Download the KRN-CJR, instructions, and scoring worksheet and receive a free KeithRN Clinical Reasoning Case Study to use with your students!
Closing Thoughts
Many programs use student predictor assessments that are designed to predict first-time NCLEX pass rates. Since passing the NCLEX does not currently ensure that a graduate nurse possesses the clinical judgment needed for safe practice (Kavanaugh & Szweda, 2017: Kavanaugh & Sharpnack, 2021), other assessments of clinical judgment are needed.
The KRN-CJR provides educators with an instrument to quantitatively assess clinical judgment to ensure safe entry into practice, resulting in improved patient outcomes.
Recommended Resources
Think Like a Nurse membership. Start practicing and develop clinical judgment skills using KeithRN Clinical Reasoning Case Studies. Access more than 300 case studies, dozens of active learning worksheets, and faculty development webinars.
Get started with an individual membership and save 50% off the first month using the discount code 50THINK.
But your best value is a program membership to get all faculty access so that your program can integrate clinical judgment resources across your curriculum. Take the next step and get a no-obligation quote!
References
- Adamson, K.A., Gubrud, P., Sideras, S., & Lasater, K. (2012). Assessing the reliability, validity, and use of the Lasater clinical judgment rubric: Three approaches. Journal of Nursing Education, 51, 66-73.
- Ashcraft, A.S., Opton, L., Bridges, R.A., Caballero, S., Veesart, A., & Weaver, C. (2013). Simulation evaluation using a modified Lasater clinical judgment rubric. Nursing Education Perspectives, 34, 122-126.
- Jensen, R. (2013). Clinical reasoning during simulation: Comparison of student and faculty ratings. Nurse Education in Practice, 13, 23-28.
- Kavanagh, J. & Szweda, J. (2017). A crisis in competency: The strategic and ethical imperative to assessing new graduate nurses’ clinical reasoning. Nursing Education Perspectives 38(2), 57-62.
- Kavanagh, J.M., Sharpnack, P.A., (January 31, 2021) “Crisis in Competency: A Defining Moment in Nursing Education” OJIN: The Online Journal of Issues in Nursing 26, No. 1, Manuscript 2.
- Lasater, K. (2007). Clinical judgment development: Using simulation to create an assessment rubric. Journal of Nursing Education, 46(11), 496-50.
- Tanner, C. A. (2006). Thinking like a nurse: A research-based model of clinical judgment in nursing. Journal of Nursing Education, 45(6), 204–211.
Keith Rischer – PhD, RN, CEN
As a nurse with over 35 years of experience who remained in practice as an educator, I’ve witnessed the gap between how nursing is taught and how it is practiced, and I decided to do something about it! Read more…
The Ultimate Solution to Develop Clinical Judgment Skills
KeithRN’s Think Like a Nurse Membership
Access exclusive active learning resources for faculty and students, including KeithRN Case Studies, making it your go-to resource.